Turquoise Claims Is Here
**Note: The Turquoise Claims process is for Medicaid claims only. All other claims should continue to be submitted through previously established processes. **
The New Mexico Health Care Authority (HCA) launched Turquoise Claims, a single-point-of-entry process for Medicaid claims, on March 23, 2026. Providers need to ensure they make changes to their Medicaid claims submission processes to avoid claim delays or denials.
Avoid Denials: What To Know
June 15, 2026: Only new Turquoise Claims payor and segment IDs will be accepted for Medicaid claims. Claims including legacy payor/segment IDs will be denied.
June 15, 2026: Medicaid claims must include a valid National Provider Identifier (NPI) and taxonomy code that match New Mexico Medicaid’s Provider Enrollment Matrix and the provider’s registered type. Providers with multiple types under one NPI must use the taxonomy code that aligns with billed services.
July 1, 2026: All ordering, rendering and prescribing providers must be individually enrolled with Medicaid to avoid claim denials. This requirement includes pharmacists, attending physicians, those practicing within group practices, hospital systems, facilities, behavioral health agencies, Indian Health Services and other organizational providers. Enroll at yes.nm.gov. To learn more, visit the HCA ORP page or view this Pharmacy Medicaid Claims Alert.
How to Ensure Accurate Claim Payment
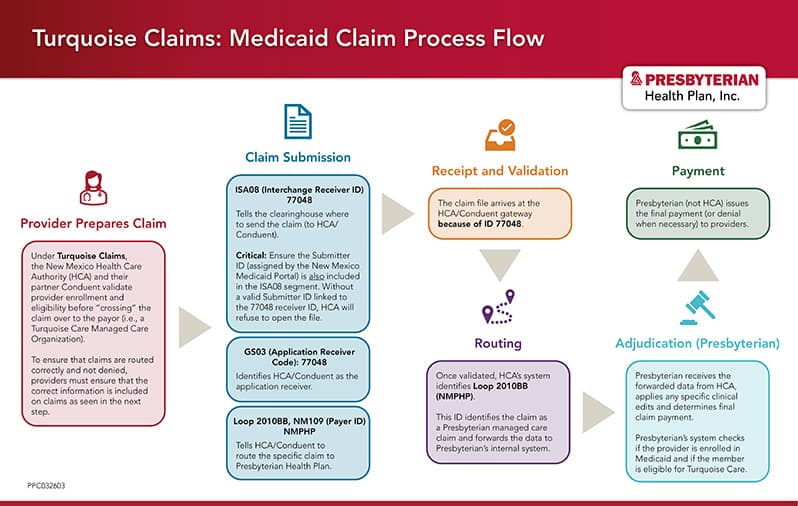
To make sure that you’re ready for Turquoise Claims, include the following on all Medicaid claims:
Presbyterian Payor ID (Segment GS03): 77048 (for PROVIDERConnect or approved clearinghouses)
Loop 2010BB (Segment NM109): NMPHP (for approved clearinghouses)
Member Information: Verify that last name/date of birth match the HCA member portal
Note: If you use an alternative clearinghouse, it is important that you contact them to provide the information above and ensure they have established a connection with Conduent and are ready to route your Medicaid claims appropriately.
Questions?
Call the Presbyterian Provider Line at (505) 923-5757 or 1-888-923-5757.


